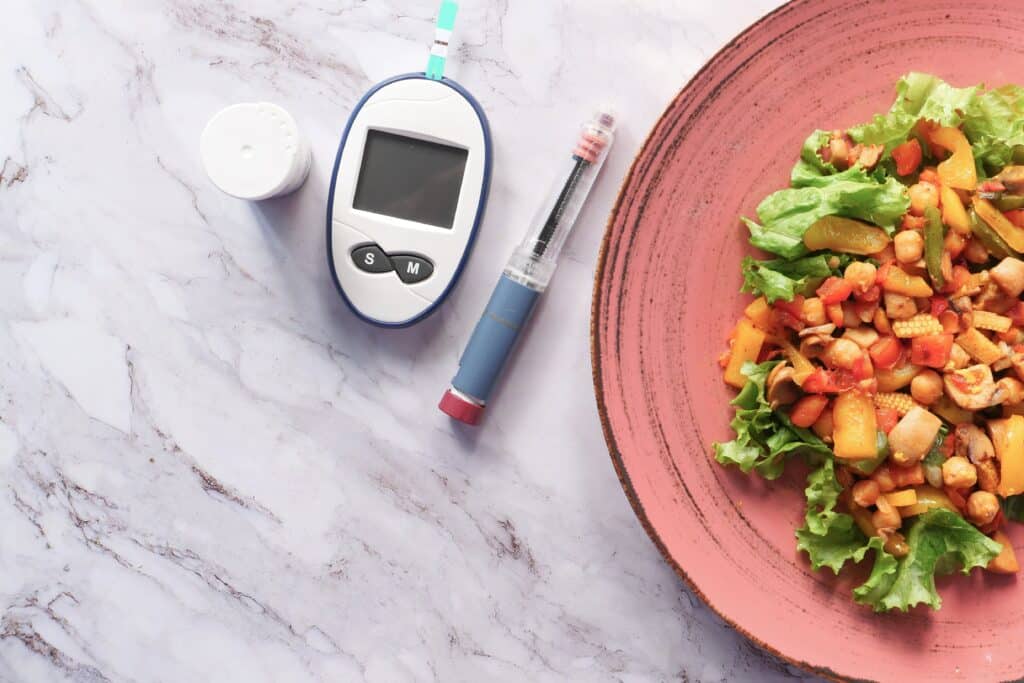HbA1c could have a significant role to play in preventing two of the leading health problems worldwide – diabetes and cardiovascular disease.

Hemoglobin A1c or HbA1c is a type of pigment in your blood that binds with glucose, which makes it a useful marker for testing people with diabetes. Regular blood tests for HbA1c levels monitor the effectiveness of diabetes management, with high levels indicating poorly controlled diabetes. Testing HbA1c is a reliable method because it represents the average levels of blood glucose over 6-8 weeks, offering a stable overview that isn’t subject to fluctuations. In contrast, the standard fasting plasma glucose (FPG) test for diabetes requires you to fast beforehand as it’s vulnerable to misleading readings after you’ve eaten.
Furthermore, a comparison of HbA1c with cholesterol levels shows there’s a significant link between HbA1c values and total cholesterol, triglyceride levels, and HDL (high-density lipoprotein) cholesterol (HDL-C), but no correlation between HbA1c and low-density lipoprotein (LDL-C) in diabetes patients. This means that it’s also possible to use HbA1c values as a predictor of dyslipidemia (high cholesterol and triglycerides) in patients who have Type 2 diabetes.
All in all, it sounds like HbA1c testing is an ideal marker; but inevitably, there’s more to it. One issue with HbA1c testing is the variation in how long red blood cells last. If a patient has anemia or other health problems like diabetes, red blood cells might survive for far shorter periods. Research suggests that people with diabetes could have red blood cell survival rates as low as 81 days, compared to 146 days in people without diabetes.
Another issue is the recommendation that 6% marks the limit – that is, no more than 6% of your total hemoglobin should be HbA1c. As long as your reading is 6% or below, conventional medicine views that as normal. Functional medicine practitioners suggest a better cut-off would be 5.3%. Who’s right? Or should the optimal HbA1c limit be even lower?
What does the evidence say about HbA1c levels?
The first issue with setting HbA1c at 6% is how close that figure is to the 6.5%, which signifies that you have diabetes. A half a percentage point isn’t a great deal when being on one side is considered healthy, while slipping across to the other is a marker for having diabetes. This margin doesn’t account for the gradual development of Type 2 diabetes, and the often prolonged stage of prediabetes, when blood sugar levels are higher than healthy but not up to the level of full-blown diabetes.
Some authorities suggest that normal HbA1c levels are below 5.7%, with prediabetes sitting in the 5.7 to 6.4% range and full-blown diabetes at 6.5%. Studies into the effects of having more than 6% HbA1c suggest that some serious complications of diabetes, like heart disease, sight loss, and kidney failure, could be prevented or at least delayed if treatment focused on keeping HbA1c levels lower than 7%. At 6% or below, HbA1c levels indicate a far lower risk of diabetic problems. Functional medicine practitioners advise an ideal range of 4.6 to 5.4%, as they say anything above 5.5% would increase your risk of diabetes. Cohen et al.’s study of HbA1c as a diagnostic tool also suggests 5.5% as a safer upper limit.
How low is too low?
Could there be health benefits to going even lower with recommended HbA1c levels? Like many substances that seem to cause health problems, such as low-density lipoprotein cholesterol (LDL-C), there could be a downside to simply trying to eliminate HbA1c. Certain research studies show a statistically significant increase in the risk of death from any cause in people with very low HbA1c levels of under 4%. So it looks like there are some health benefits to having a small percentage of HbA1c in your blood, although what these might be is still unclear.
What’s the optimal level of HbA1c?
As the current 6% upper limit is set so close to the 6.5% that indicates diabetes, it makes sense to re-evaluate that limit. Given that the turning point for the adverse effects of too little HbA1c is around 4%, and functional medicine advises HbA1c be in the range of 4.6% to 5.3%, a sensible marker might be a target of 5%.
How do I lower my HbA1c?
Diet plays a big part in reducing your HbA1c levels. A high intake of refined carbohydrates like white bread, white rice, cookies, and other processed foods is one of the leading causes of elevated HbA1c, so you should avoid these as much as possible. Go for unrefined carbohydrates that are still full of fibre, vitamins, and minerals, such as whole grains, fruits, vegetables, and beans, but try not to exceed 45 grammes per meal.
Excessive intake of any type of food could raise your HbA1c levels, so watch your portion sizes for fats and protein as well. Combine these dietary changes with increased physical activity, and you should achieve a reduction in HbA1c.
One other issue to bear in mind when looking at the links between HbA1c and cholesterol is the potential for an inflated score if you already have the genetic condition
hypertriglyceridemia. This condition artificially raises the blood test reading for HbA1c, so you need to be aware of this possible complication.
Overall, HbA1c offers a convenient and reasonably accurate indication of your risk of both Type 2 diabetes and cardiovascular disease. Aiming for levels no higher than 5% looks like the best way of avoiding these major health conditions and the complications they cause.