Essential hypertension, characterised by persistently high blood pressure with no clear underlying cause, poses a significant health risk worldwide. It is a condition that can act as a silent killer, striking without warning unless the lifestyle issues contributing to it are properly addressed. Managing essential hypertension is not just vital; it’s a life-saving endeavor that requires a deep understanding of its potential causes—from insulin resistance and sleep apnea to nutrient deficiencies—and the implementation of effective lifestyle and dietary strategies.
In this comprehensive guide, we delve into the critical aspects of managing essential hypertension, combining valuable insights and practical advice to help you learn about the underlying causes and implement key strategies, thus averting the risks associated with this common yet often underestimated health threat.
What is Essential Hypertension
Essential hypertension is a condition where the force of the blood pumping through your arteries reaches a dangerous level. Having hypertension substantially increases your risk of developing numerous health problems, including atherosclerosis (narrowed arteries), heart disease, stroke, aneurysms, retinal damage in the eyes, and kidney disease.
Around three-quarters of the people who suffer a stroke or heart attack each year have hypertension, so the disease presents a serious health risk; unfortunately, rates of hypertension worldwide are generally on the rise.
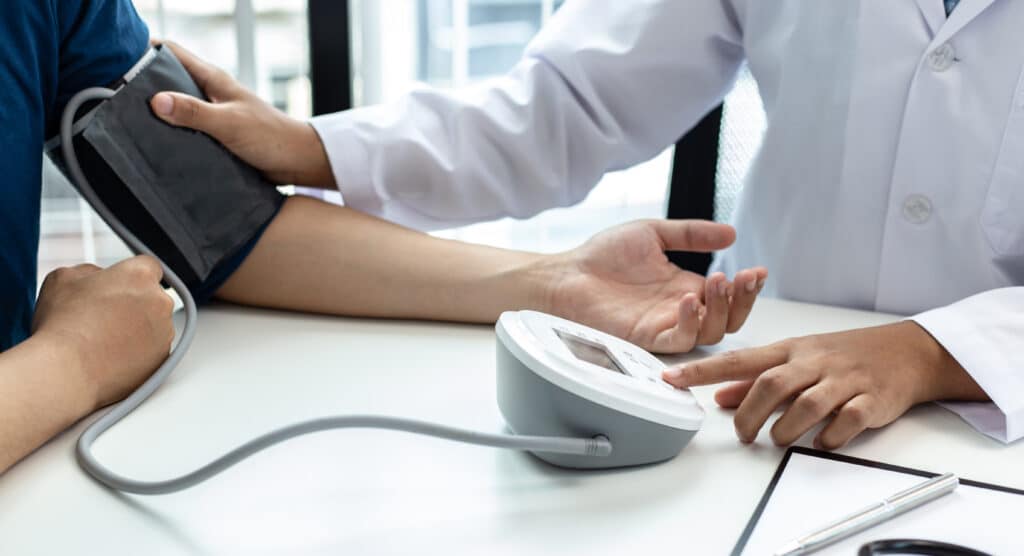
How is Blood Pressure Measured?
You’re probably familiar with the blood pressure test, as it’s one your doctor or other health care professional is likely to perform when you’re sick or as part of a routine checkup. The blood pressure cuff goes around your arm, your doctor inflates it, then records the pressure in the arteries when your heart’s beating and in between beats.
The beating heart reading is the systolic measurement, while the reading between beats is the diastolic measurement. In combination (systolic over diastolic), these readings give you your blood pressure. The results can be summarised as follows:
- Normal blood pressure: Below 120 systolic and 80 diastolic.
- Elevated blood pressure (pre-hypertension): 120-129 systolic and below 80 diastolic.
- Stage 1 hypertension: 130-139 systolic, 80-89 diastolic.
- Stage 2 hypertension: 140 or higher systolic, 90 or higher diastolic.
There are two types of hypertension. Secondary hypertension arises from a specific underlying disease state, most commonly kidney disease and endocrine disorders. Essential hypertension occurs independently of a specific disease. Conventional medicine often refers to essential hypertension as idiopathic, meaning it has no definable cause; but functional medicine practitioners have identified many likely causes and triggers for essential hypertension.

What Causes Essential Hypertension?
The causes of essential hypertension proposed by functional medicine include:
Increasing age
Age plays a part in the development of essential hypertension because of the arterial stiffening that occurs as you get older.
Obesity
Obesity is known to be a key risk factor for hypertension. However, not all people who are obese will have high blood pressure, and hypertension can affect people with a supposedly healthy BMI (body mass index).
Sympathetic nervous system activity
Emotions such as stress, repressed anger, and anxiety all increase the activity of your sympathetic nervous system. This leads to the repeated release of hormones like adrenaline that prime your body to escape from or confront danger (the fight-or-flight response).
Poor Diet & Nutrient Deficiency
A diet that’s high in salt and sugar and/or low in fibre increases your risk of developing essential hypertension. Micronutrient deficiencies such as a lack of potassium and/or magnesium, are also significant. There’s evidence to suggest that a lack of vitamin D could also contribute to essential hypertension.
Unhealthy habits
Drinking too much alcohol, smoking, or having more than five drinks containing caffeine each day all increase your risk of essential hypertension.
Physical Inactivity
You might not be overly surprised to hear that an inactive lifestyle is a risk factor for hypertension, and how this contributes to low nitric oxide production which dilates blood vessels. However, you might be less aware that excessive exercise can also adversely affect your blood pressure.
Insulin Resistance
People with insulin resistance often have high blood pressure. The raised blood glucose levels typical of insulin resistance can damage your blood vessels, causing several serious circulatory problems of which hypertension is just one.
Exposure to toxins
Excessive or cumulative contact with heavy metals like lead, or exposure to toxic chemicals, could increase your risk of getting essential hypertension.
Obstructive Sleep Apnea
Obstructive sleep apnea affects your sleep. During the night, you stop breathing when soft tissues in the back of your throat relax too far and cut off the air supply. Your brain responds by waking you up, but as this can occur multiple times in one night, your blood oxygen levels fall, and you can develop nocturnal hypertension. This affects your sympathetic nervous system, which alongside oxidative stress, inflammation, and nitric oxide release, may lead to sustained daytime hypertension.
Genetic Predisposition
Like many aspects of your health, the genes you inherit from your parents could influence your risk of developing essential hypertension.
High homocysteine levels
Homocysteine is an amino acid, one of the components of all proteins in your body. Factors like a high caffeine intake, stress, and a lack of B vitamins all contribute to high homocysteine levels – a risk factor for increased systolic pressure.
Understanding the intricate causes behind essential hypertension is the first critical step towards safeguarding your health against this silent threat.
By pinpointing these underlying factors, functional medicine practitioners empower you with the knowledge needed to make informed decisions about your health journey.
Stay informed, and consult with healthcare professionals to explore personalised strategies for maintaining optimal blood pressure levels and overall well-being. If you have any concerns or are seeking more individualised advice, book a free consultation with us. We can help you on your journey to better health.